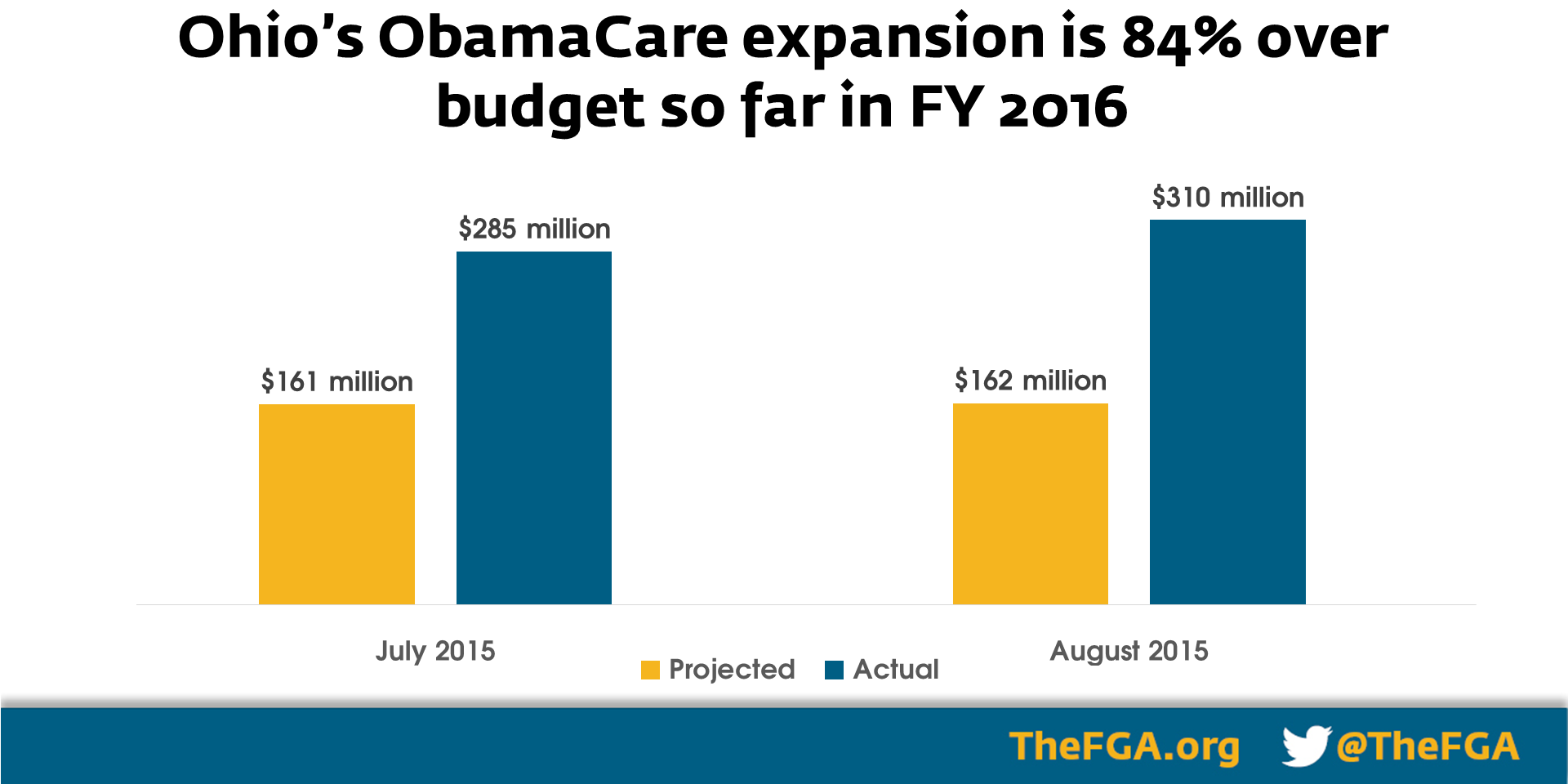
So, got this in email the other day:
"A new ratings system created by the National Committee for Quality Assurance (NCQA) provides consumers with a more accurate picture of how health insurance plans perform in key quality areas."
That's (mildly) interesting, but what were those "key" areas?
Oh:
"[C]linical quality, member satisfaction and NCQA Accreditation Survey" [emphasis added]
Are you kidding? One third of the metric is itself?
How does that work?
More importantly, though, is the self-delusion that consumers actually care about these kinds of things:
"Oh sure, Anthem has a terrific rate, $100 a month cheaper than Humana, but Humana ranks 3 spots higher on NCQA, so I'll go with them."
Said no one, ever.
It's similar to the experts who claim that folks inadvertently "leave money on the table" by not choosing a health insurance plan that offers cost-sharing in addition to premium subsidies. There's a reason, and it's not ignorance of the program.
It's human nature.
"A new ratings system created by the National Committee for Quality Assurance (NCQA) provides consumers with a more accurate picture of how health insurance plans perform in key quality areas."
That's (mildly) interesting, but what were those "key" areas?
Oh:
"[C]linical quality, member satisfaction and NCQA Accreditation Survey" [emphasis added]
Are you kidding? One third of the metric is itself?
How does that work?
More importantly, though, is the self-delusion that consumers actually care about these kinds of things:
"Oh sure, Anthem has a terrific rate, $100 a month cheaper than Humana, but Humana ranks 3 spots higher on NCQA, so I'll go with them."
Said no one, ever.
It's similar to the experts who claim that folks inadvertently "leave money on the table" by not choosing a health insurance plan that offers cost-sharing in addition to premium subsidies. There's a reason, and it's not ignorance of the program.
It's human nature.